In the U.S., 1 in 5 people have diabetes, and estimates suggest an additional 8.5 million Americans have diabetes but haven’t yet been diagnosed. Certain racial and ethnic groups have a higher risk of developing diabetes. The Centers for Disease Control and Prevention reports these percentages of adults with diabetes in the U.S. by race and ethnicity in 2018-20191:
| Race and Ethnicity | Percentage |
| American Indian or Alaska Native | 14.5 |
| Asian, non-Hispanic | 9.5 |
| Black, non-Hispanic | 12.1 |
| Hispanic, overall | 11.8 |
| White, non-Hispanic | 7.4 |
A lack of insurance coverage and fewer years of education are shown to be factors in this racial and ethnic disparity. Improving the quality of and access to diabetes care for marginalized groups can help reduce rates of diabetes complications, healthcare costs, and deaths.2,3
Improving Diabetes Care for Underserved Communities
The American Diabetes Association (ADA) issued guidelines in January 2023 for standards of care for people with diabetes. For underserved communities, the ADA recommends:
- Assess food, nutrition, housing, and financial status and refer to local community resources when necessary.
- Screen for diabetes and cardiovascular disease. As needed, involve community health workers to support the management of these diseases.
- Provide ongoing self-management support from health coaches and community health workers when available.4
Standards of Care for Diabetes: Developing Rapport and Addressing Patient Needs
Healthcare professionals (HCPs) can establish rapport by asking questions to assess the needs of their patients and offer realistic solutions. Many people experiencing financial insecurity also experience food and nutrition insecurity, unstable housing, an inability to store refrigerated medications correctly, and transportation issues.
Below is a list of questions that HCPs could consider asking, along with ways to take action in supporting their patients with diabetes:
Health literacy
- Ask: Do you have questions about why the medications you take and the food you eat affect your diabetes?
- To Do: This conversation starter can help HCPs provide additional resources and practitioner recommendations for accessible information about diabetes care.
Food and nutrition security
- Ask: Have you ever worried about running out of money to buy food, or is it currently a struggle for you to buy food?
- To Do: Have a list of local resources for food and consider recommending food prescription programs, federal food assistance programs, and recommendations for local food pantries, as needed.
Adherence to prescribed medication and testing regimen
- Ask: Have you ever run out of money to buy your medications or testing supplies?
- To Do: Track medication and testing behaviors of clients and have an intervention plan for non-compliance due to financial constraints. Offer cost-effective alternatives for medication and testing supplies and virtual visits as necessary to answer questions and help them get back on track with the prescribed regimen.4
- Ask: Do you have concerns about your medications?
- To Do: Recognize and acknowledge fears about starting certain medications and provide plain-language support to follow the HCP recommendations.5
Cultural Sensitivities in Counseling
When counseling patients, it’s imperative to consider cultural sensitivity and humility in communication.
As aAs an expert who regularly counsels clients, Orgain Nutrition Advisory Board Member and Certified Diabetes Care and Education Specialist Kim Rose, RDN, CDCES, CNSC, LD, states: “Instead of labeling a person as a ‘diabetic,’ say someone living with diabetes.”
- Rose says to refrain from using difficult medical jargon. “Many patients need help understanding their test results, medication pamphlet inserts, and even what their HCPs say. Educate your clients on common terms used in the diabetes space. Consider starting with glucose, hyperglycemia, hypoglycemia, glycated hemoglobin (HgA1C), and cardiovascular complications.”
- Reiterate concepts using the client’s words. “Reflect on comments made by your patient or client to show that you are listening and to ensure you correctly understand what is being communicated,” says Rose.
- Speak slowly and clearly. “Use open-ended questions to establish rapport, spark discussion, and examine beliefs, attitudes, and values related to food, nutrition, and diabetes,” Rose adds.
- Be specific with advice. For example, instead of stating to test your blood sugar in the morning and at night, give particular times that match the client’s schedule.
- Use graphics and pictures to describe essential concepts.
- Demonstrate how to test blood sugar, choose foods, or plan meals whenever possible.
- Invite the client to tell you what they have learned. Confirm understanding and address any gaps in knowledge.6
Customizing the Diabetes Plate Method
It can be common for HCPs to recommend a style of eating that does not fit within the client’s cultural food preferences. However, a critical component of dietary adherence is carefully assessing each client’s eating habits before making nutritional recommendations.7 When possible, gather a three-day written food recall and smartphone images of meals8, but when this isn’t possible, take time to identify typical foods eaten before making recommendations.5
The diabetes plate method The diabetes plate method (DPM) can capture cultural food preferences, and HCPs will often need to take small steps toward achieving these types of portions. The DPM uses a nine-inch plate with half filled with non-starchy vegetables and the other half split evenly between carbohydrate-rich foods and protein-rich foods with water or a non-calorie beverage to drink.9 For vegetarian diets, half of the plate can be filled with non-starchy vegetables, and the other half can include a combination of foods with carbohydrates and protein, such as fruit, grains, beans, dry peas, lentils, and soy.10 Orgain vegan protein powders are a great way to include protein in any meal.
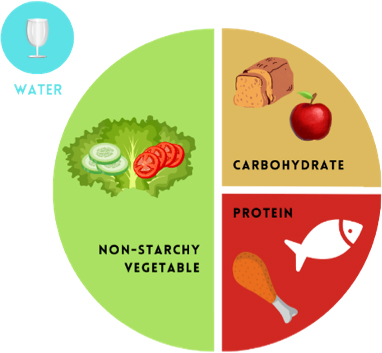
When addressing culturally inclusive food recommendations, it’s essential for the HCP to consider several factors, including:
- Affordability – Many people perceive fruits and vegetables to be more expensive.11 Explore ways to direct clients to low-cost, culturally appropriate produce such as fresh produce in season or on sale, frozen, plain vegetables, and fruit, canned in water, and dehydrated vegetables. Encourage clients to eat fresh produce first before it goes bad.
- Temper expectations – Some people expect immediate results from changing eating habits. Guide clients about the long-term benefits of following recommended practices.12
- Easy access to nutrient-poor foods in food deserts – Inquire about retailer access and consider transportation and cost for recommended foods.11,12 Explore options available at dollar stores or big-box retailers if there is no nearby grocery store.
- Address adherencein follow-up visits – New challenges can arise, so be ready to address non-adherence with eating habits using compassion and realistic solutions.6
Orgain Diabetes-Friendly Products and Professional Education
Orgain offers a wide variety of diabetes-friendly nutrition products made with clean ingredients and designed to fit the changing needs of your patients and clients. With a wide variety of ready-to-drink shakes and protein powders, Orgain offers delicious products boasting an impressive nutrition profile, including zero or minimal added sugar, low total carbohydrates, and high protein. Here are a few of many Orgain products that healthcare professionals most often recommend to their patients with diabetes, along with nutritional highlights:
- Organic Protein™ Plant-Based Powder
- 0g total sugar, 15g carbs, and 21g protein
- 20-gram Plant-Based Protein Shake
- 0g total sugar, 8g carbs, and 20g protein
- 26g Organic Protein Grass Fed™ Protein Shake
- 1g total sugar, 15g carbs, and 26g protein
- Organic Protein™ Superfoods Plant-Based Protein Powder
- 1g total sugar, 20g carbs, and 21g protein
Orgain’s Healthcare Ambassadors can send Orgain product samples to patients through the Ambassador Sampling Portal. If you’re not a healthcare ambassador yet, request an account now. Once approved, visit the Ambassador Sampling Portal to send samples to your patients.
Here are some of Orgain’s popular educational resources on diabetes:
Professional Education Webinar Series:
Individualizing Nutrition for Type 2 Diabetes: Out with the Old, In with the New, presented by Angela Manderfeld, MS, RD, CDCES, BC-ADM
(Released: 11/11/21)
The Good Clean Nutrition Podcast
Episode 19: Managing Diabetes & The Road to Better Blood Sugar Control with Kim Rose, RDN, CDCES, CNSC, LD
(Released: 11/17/22)
Science-Based Brief
Exploring a Personalized Approach to Type 2 Diabetes Management
(Published: 11/04/22)
Using the Latest Technology to Monitor and Manage Blood Glucose
(Published: 11/11/21)
References:
- Centers for Disease Control and Prevention. By the Numbers: Diabetes in America. Available at: https://www.cdc.gov/diabetes/health-equity/diabetes-by-the-numbers.html
- Canedo JR, Miller ST, Schlundt D, Fadden MK, Sanderson M. Racial/Ethnic Disparities in Diabetes Quality of Care: the Role of Healthcare Access and Socioeconomic Status. J Racial Ethn Health Disparities. 2018 Feb;5(1):7-14. doi: 10.1007/s40615-016-0335-8. Epub 2017 Jan 11. PMID: 28078660; PMCID: PMC5505804.
- Lucero JE, Roubideaux Y. Advancing Diabetes Prevention and Control in American Indians and Alaska Natives. Annu Rev Public Health. 2022 Apr 5;43:461-475. doi 10.1146/annurev-publhealth-093019-010011. PMID: 35380066; PMCID: PMC9924140.
- ElSayed NA, Aleppo G, Aroda VR, Bannuru RR, Brown FM, Bruemmer D, Collins BS, Hilliard ME, Isaacs D, Johnson EL, Kahan S, Khunti K, Leon J, Lyons SK, Perry ML, Prahalad P, Pratley RE, Seley JJ, Stanton RC, Gabbay RA, on behalf of the American Diabetes Association. 1. Improving Care and Promoting Health in Populations: Standards of Care in Diabetes-2023. Diabetes Care. 2023 Jan 1;46(Supple 1):S10-S18. doi: 10.2337/dc23-S001. PMID: 36507639; PMCID: PMC9810463.
- Caballero AE. The “A to Z” of Managing Type 2 Diabetes in Culturally Diverse Populations. Front Endocrinol (Lausanne). 2018 Aug 28;9:479. doi: 10.3389/fendo.2018.00479. PMID: 30233490; PMCID: PMC6127640.
- U.S. Department of Health and Human Services. Think Cultural Health. Providing CLAS. Available at: https://thinkculturalhealth.hhs.gov/assets/pdfs/resource-library/providing-clas.pdf
- Duffy, L., & Burt, K. G. (2020). Exploring the Relationship between Cultural Humility and Professional Diversity through the Biased Mediterranean Diet. Journal of Best Practices in Health Professions Diversity, 13(2), 174–183. https://www.jstor.org/stable/27056499
- Six BL, Schap TE, Zhu FM, Mariappan A, Bosch M, Delp EJ, Ebert DS, Kerr DA, Boushey CJ. Evidence-based development of a mobile telephone food record. J Am Diet Assoc. 2010 Jan;110(1):74-9. doi: 10.1016/j.jada.2009.10.010. PMID: 20102830; PMCID: PMC3042797.
- American Diabetes Association. Try the Diabetes Plate Method. Available at: https://diabetes.org/food-nutrition/eating-healthy
- Jardine MA, Kahleova H, Levin SM, Ali Z, Trapp CB, Barnard ND. Perspective: Plant-Based Eating Pattern for Type 2 Diabetes Prevention and Treatment: Efficacy, Mechanisms, and Practical Considerations. Adv Nutr. 2021 Dec 1;12(6):2045-2055. doi: 10.1093/advances/nmab063. PMID: 34113961; PMCID: PMC8634508.
- Cortés DE, Millán-Ferro A, Schneider K, Vega RR, Caballero AE. Food purchasing selection among low-income, Spanish-speaking Latinos. Am J Prev Med. 2013 Mar;44(3 Suppl 3):S267-73. doi 10.1016/j.amepre.2012.11.012. PMID: 23415192.
- Breland JY, McAndrew LM, Gross RL, Leventhal H, Horowitz CR. Challenges to healthy eating for people with diabetes in a low-income, minority neighborhood. Diabetes Care. 2013 Oct;36(10):2895-901. doi: 10.2337/dc12-1632. Epub 2013 Jul 22. PMID: 23877980; PMCID: PMC3781525.



